
Plantar Fasciitis Exercises: The Complete Guide to Relieving Heel Pain and Preventing Recurrence
If you are searching for plantar fasciitis exercises, you are likely dealing with persistent heel pain that is affecting your ability to walk, train, or even get through the day comfortably. For many people, the pain is most noticeable with the first steps in the morning or after long periods of sitting, and it can gradually worsen if not managed correctly.
The key point to understand early is that plantar fasciitis is not just a simple “tightness” problem. It is typically the result of excessive load being placed on the plantar fascia without the necessary strength, mobility, or recovery to support it. This is why exercises are among the most effective treatments when applied correctly and progressed appropriately over time.
At Burleigh Central Physiotherapy, we regularly see patients who have tried generic stretches found online with limited success. The difference between short-term relief and long-term resolution usually comes down to understanding how to combine stretching, strengthening, and load management into a structured plan.
Understanding Plantar Fasciitis and Why Exercise is Essential
The plantar fascia is a thick band of connective tissue that runs along the bottom of your foot, connecting the heel bone to the toes. Its role is to support the arch of the foot and absorb forces during walking, running, and standing.
When the load placed on this structure exceeds its capacity, small areas of irritation and degeneration can develop. This leads to classic symptoms of plantar fasciitis, including sharp heel pain, stiffness, and reduced activity tolerance.
Exercises are essential because they directly address the root causes of the condition. Stretching improves flexibility in the calf and foot structures, reducing tension on the fascia. Strengthening exercises increase the capacity of the muscles and tissues to handle load. Together, these changes allow the plantar fascia to recover while also reducing the likelihood of future flare-ups.
The Most Effective Plantar Fasciitis Exercises
Calf Stretch (Straight Leg)

Tightness in the calf muscles is one of the most common contributing factors to plantar fasciitis. When the gastrocnemius muscle is restricted, it limits ankle movement and increases strain through the foot.
This stretch should be performed slowly and consistently, with the back leg kept straight and the heel firmly on the ground. Over time, improved calf flexibility can significantly reduce stress on the plantar fascia during walking and standing.
Bent-Knee Calf Stretch (Soleus Stretch)
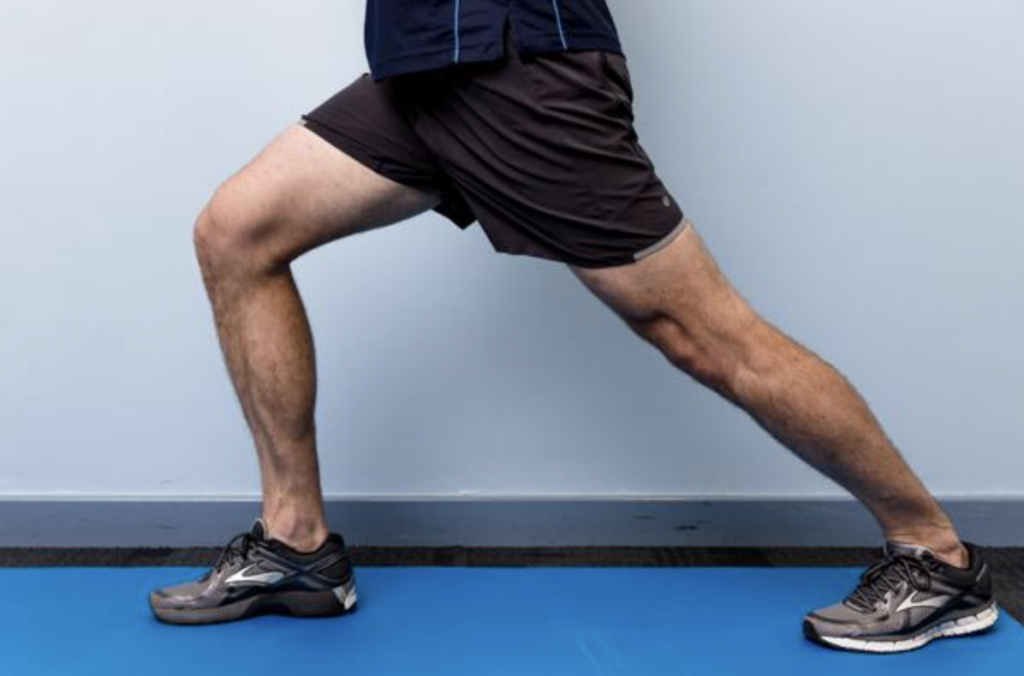
The soleus muscle sits deeper in the calf and plays a major role in everyday activities such as walking. It is often overlooked in rehabilitation programs, yet tightness here can continue to drive symptoms even when other stretches are being performed.
By bending the back knee while maintaining heel contact with the ground, this stretch targets the deeper muscle fibres and improves overall ankle mobility, which is critical for reducing compensatory stress through the foot.
Plantar Fascia Stretch
Directly stretching the plantar fascia can help reduce morning pain and stiffness. This is particularly effective when performed before taking your first steps of the day.
By pulling the toes back toward the shin, tension is applied along the length of the fascia, helping to maintain tissue flexibility and reduce the sharp pain often experienced with initial weight-bearing.
Foot Strengthening Exercises
Strengthening the small muscles within the foot is often neglected, yet these muscles play a key role in supporting the arch and distributing load effectively.
Exercises such as towel scrunches or controlled toe movements help improve stability and reduce reliance on passive structures like the plantar fascia. Over time, this improves foot mechanics and reduces strain during daily activities.
Heel Raises and Load Progression
Heel raises are one of the most important components of a successful rehabilitation program. They help build strength in the calf and foot complex, increasing the tissues’ ability to tolerate load.
Starting with both feet and progressing to single-leg variations allows for gradual adaptation. Slower, controlled movements—particularly during the lowering phase—are especially effective in improving tissue resilience.
This progression is often the difference between temporary relief and full recovery.
Common Pitfalls That Delay Recovery
Many people experience prolonged symptoms not because the condition is severe, but because their treatment approach is incomplete or inconsistent.
A common mistake is relying solely on stretching without incorporating strengthening exercises. While stretching can provide temporary relief, it does not increase the tissue’s capacity to handle load, which is essential for long-term improvement.
Another issue is inconsistency. Exercises need to be performed regularly and with proper technique to be effective. Sporadic effort often leads to minimal results and ongoing frustration.
Ignoring footwear is another major factor. Shoes that lack support or have worn-out cushioning can continue to aggravate the condition, even if exercises are being performed correctly.
Finally, many people fail to progress in their exercises. As the body adapts, the level of load must increase to continue improving strength and resilience. Without progression, recovery can plateau.
How Long Does It Take to Recover?
Recovery timelines vary depending on the severity of the condition and the timing of appropriate treatment. In general, most people notice some improvement within the first few weeks of regular exercise.
However, full recovery often takes several weeks to a few months. This is because the plantar fascia requires time to adapt to increased load and rebuild its capacity.
Patience and consistency are critical. Attempting to rush the process or returning to high-impact activities too early can lead to setbacks.
When to Seek Professional Advice
While exercises are highly effective, they are not always sufficient on their own. If symptoms persist despite consistent effort, it may indicate underlying factors that require further assessment.
These can include biomechanical issues, gait abnormalities, or specific strength deficits that are not being addressed with general exercises.
At Burleigh Central Physiotherapy, we take a comprehensive approach to treating plantar fasciitis. This includes assessing movement patterns, identifying contributing factors, and developing a tailored program that aligns with your lifestyle and activity goals.
The Right Next Step
Plantar fasciitis can be a frustrating and persistent condition, but with the right approach, it is highly manageable and often fully reversible.
Understanding which exercises to perform, how to progress them, and how to avoid common mistakes can significantly reduce recovery time and improve long-term outcomes.
If you are based in Burleigh Heads and want a clear, structured plan for plantar fasciitis exercises, contact Burleigh Central Physiotherapy on (07) 5576 0747 to take the next step toward recovery.

